

How politics affected digital healthcare in the USA
Quality of care services and their costs are the main aspects of care people are interested in.
The history of American healthcare can be described as the governments’ attempt to come up with a solution that will satisfy medical communities, employers, insurers, patients and worker unions behind them. Quiet challenging task, if not unrealistic.
The inability to find the said solution defined the state of the industry: the USA is the only developed country without universal insurance coverage; healthcare spending here is highest among America’s peers; healthcare is a top issue Americans care about: 36% ranked it first, and 26% listed it second in RealClear Opinion Research’s survey of 2019. And it’s been happening for a long time…

Digital healthcare is an integral part of the industry now: technologies are changing the way care is received, delivered, and performed. Hospitals use EHRs to manage health data. Patients use their smartphones and wearables to manage and monitor their health. Healthcare organizations make deals with tech vendors to increase their value with innovations and optimize internal processes.
Digital healthcare became a part of the industry and inherited its regulations, obligations, and heavy dependency on the government’s views.
The early history of digital healthcare: the becoming of HIMSS
In 1952, the American Hospital Association (AHA) started its Committee on Methods improvement. The same year, the University of Connecticut hosted the first workshop on simplifying the way the hospital works. On the other side of the country, Earl J. Frederic became the first hospital management engineer.
That year laid a foundation for changing approach to hospital management. The new approach was supposed to save costs for hospitals and improve the quality of their services. “Hospital management engineer” became a profession as hyped as today’s data scientists. The difference between “engineers” and usual hospital administrators was in organized, evidence-based and executed with clinicians’ help way of managing. Eventually, the AHA persuaded hospital administrators to adopt the approach.
Those who believed in efficiency and profitability of this approach started Hospital Management Society (HMSS), a non-profit volunteer organization aimed at improving the design of hospital systems, hospital management and administration processes. They provided education for those who wanted to improve the way hospitals perform and held annual conventions with people from providers, businesses, and other organizations who were management engineers or wanted to adopt the position for themselves. HMSS worked in parallel with the AHA, that had its own way of promoting “methods improvement” across hospitals, and in 1966, they’ve affiliated.
Soon, with information technologies emerging, HMSS became HIMSS (Healthcare Information and Management System Society) and started to accept and educate technology specialists for the healthcare industry. When the AHA cut its workforce due to the nineties crisis, HIMSS gained independence. During its history, Society published lots of papers introducing medical professionals to new management approaches and, then, new technologies; among other things, its members started popularizing CIO position and its value for hospitals.
In 1993, Bill Clinton presented the Health Security Act with a section on the role of information system. 1993 is a year when healthcare information legislation started to pop up: to develop large health information networks to fasten healthcare administration and finances; to pilot telemedicine projects; etc.
The nineties started a talk on healthcare automation via technology. Bill Gates, James Buckley, and Charles Wang attended the HIMSS conference in 1995. Next year, HIMSSLIST, an Internet email service, was introduced to an organization for HIMSS members to exchange ideas over the web.
HIMSS formed a lot of alliances, partnerships, and synergies: all to share knowledge on new hardware, software and on how to adapt and use it in hospitals. In 2004, they also founded Certification Commission for Health Information Technology, which, until 2014, was an authorized tester and certifier for electronic health records.
Basically, that is what HIMSS is doing now: they promote information technologies to improve health outcomes and make healthcare more cost-effective for hospitals. HIMSS members are over 600 corporations, 350 non-profit organizations, and more than 55,000 individuals. More than half of HIMSS members work as healthcare providers.
One of the things HIMSS was doing at the beginning of this century is educating healthcare providers on HIPAA.
HIPAA, HITECH, and EHRs and Obama’s Administration
HIPAA legislation was signed into law by Clinton in 1996. We talked explicitly about why it’s important for digital healthcare businesses to comply with the regulations.
Initially, HIPAA was a legislation that was aimed at improving “portability and accountability” of health insurance: insurers could transfer employees’ insurance packages when they changed jobs. Also, low promoted medical savings through tax breaks and coverage for people with pre-existing conditions. Then, it transformed into a law that protects patients’ privacy and access to their data through obliging organizations to install safeguards and train staff on security.
To simplify transitions and administration of health insurance data, healthcare industry started to digitize patient information. The tech programs were regulated by HIPAA, as well. The government also saw the potential of digitization for hospitals and patients.
Thus, in 2009, Barack Obama signed into law the Health Information Technology for Economic and Clinical Health Act — HITECH Act — and introduction of Meaningful Use incentive program. The Act gave money to providers who adopted health IT solutions and penalize those who didn’t. In this way, utilization of EHRs grew from 9% of hospitals in 2008 to 96% of hospitals in 2015. (Nice.)
In 2013, OCR released the Omnibus Final Rule for HIPAA. It required not only providers, clearinghouses, and other organizations who work directly with patients’ private info to comply with HIPAA, but any of their business associates who interact with patients’ data in any way.
After the release of the Final Omnibus Rule, a lot of healthcare organizations improve their security because of large and scary penalties of HIPAA violations.
The HITECH Act started a new era: with almost mandatory digitization, a lot of software vendors got the opportunity to participate in the process of making healthcare more comfortable.
EHRs systems could be connected to other solutions (for instance, to smartphones and wearables — making healthcare more accessible), digitized data became a source of raw material for data analytics and building machine learning algorithms, customers get an opportunity to schedule visits via internet and reduce the communication gap with doctors.
At the same time, HIMSS and organizations like it started collaborating in the efforts to pursue interoperability.
Affordable Care Act and Digital Health
President Obama signed a document that will be called Obama Care on March 23, 2010. According to this new healthcare law - Patient Protection and Affordable Care Act— every American should have insurance. Insurance coverage was meant to be funded from taxes.
More than 200 million Americans gained insurance under the ACA. As a part of the ACA’s requirements, 37 states expanded Medicaid, providing coverage for the vulnerable population; these people finally got access to healthcare. The act reduced healthcare spending per person via Medicaid, simultaneously allowing to bring up more people onto coverage.
The ACA started the first health insurance marketplace - and, politically, started the trend of shopping for insurers: people could sign up for a certain package and apply for federal subsidies for that package.
Act was created to drive the market to the creation of new solutions, that will help improving health outcomes without increasing services’ costs: the ACA opened the way for funds going into digital health.
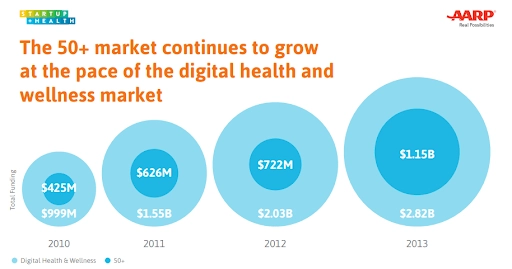
For instance, it gave a push to the development of connected technologies for healthcare, especially telehealth, — as telemedicine is basically an epitome of affordable, accessible care of high quality, which was the cornerstone of the Act. Markets of solutions for an ageing population, healthcare navigation, emergency detection, fitness, etc, also grew.
The ACA also prohibited insurers to deny their services to people with pre-existing or chronic conditions, and that gained the pact popularity among both American parties.
On the less bright side, the ACA didn’t allow health insurers to include caps on lifetime benefits: if people were seriously ill or if a child was born sick, there was no life support for their health. On the other hand, people who weren’t seriously ill, didn’t have to pay for it…
Under the ACA, Medicaid stopped paying for hospital-acquired infections and they began to treat and prevent them (and charge accordingly.)
Obama Care was, in general, good for people, but a bit raw — in terms of its goals. Thousands of Americans stayed uninsured. Cost of healthcare services wasn’t reduced: so, while everyone could get insurance — it often still wasn’t enough, because no one worked with the cost of health services.
While Medicaid, expanded under the ACA, and the ACA itself improved the lives of Americans, and digital adoptions driven with HITECH opened some large opportunities for startups and vendors in the fresh filed, the efforts we’ve been talking about in the second paragraph, the awareness and education efforts on new technologies lacked. That resulted in lots of confusion among clinicians.
Trump Administration and Digital Health
The ACA was transformed and weakened in 2017 by Donald Trump’s administration. They stopped reimbursements for insurers who paid for deductibles and copayments for six million residents with low income, so insurers raised their rate — and the raise was approved by few states.
The same year, Trump administration allowed private insurance companies to sell policies across different states, which made it harder for a federal insurer to operate across the country. The plan was to increase competition and lower prices, but, as expected, the opposite happened: those private companies who really could operate across the states increased their prices because of increased influence in the market.
President Trump eased restriction of short-term plans, wanting them to last up to 12 months. He also announced cutting near 10.4$ billion from insurers, efficiently taking away most of their subsidiary finances. Which also allowed them to raise plans’ cost - according to the Urban Institute, by 18%.
In 2018, States were given permission to require employment from people under Medicaid, and 18 states used that permission. New “public charge” rule will allow denying citizenship to immigrants who are on Medicaid.
Trump also cancelled the ACA’s requirements to penalize those who don’t have insurance — which, as you can guess, is good, if you’re healthy.
While things are pretty bad for people with low income, without jobs, and with chronic conditions, they were (and are) kind of good for business.
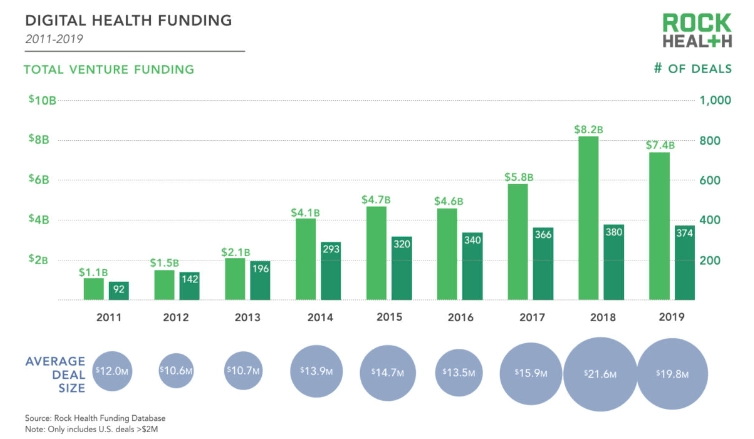
Trump encouraged new technologies and digital health businesses. In 2017, he signed a bill that reauthorised the FDA’s user fee agreement for drug and devices. The bill gave funds to digital health unit of the FDA and allowed them to use more new data sources. Bill laid out new approaches to digital health: for instance, the establishment of a central digital health unit within CDHR (Center for Devices and Radiological Health).
Trump also announced a public health emergency related to “opioid crisis.” President’s report on combating drug addiction encourages more digital tech to address it at the beginning of 2018. In his plans for 2020, he announced there will be more funds for wearables and other medical devices.
Finally, Trump did an unprecedented thing for American healthcare: recently, he signed a regulation that will require hospitals to be transparent about their prices and list 300 “shoppable” services on their site. According to this regulation, insurers will also be required to be very specific about how much they will compensate for a certain procedure and how much patients would have to pay from their pocket. Good for app developers, not so black-and-white for physicians and patients.
Conclusion - politics and digital healthcare in the USA
We can’t help, but notice that the majority of politicians’ efforts in regulating healthcare spendings and increasing health coverage doesn’t exactly deal with… providers. We called Trump’s requirements to establish transparent healthcare prices unprecedented because it’s the first move in American history where providers are required to do something with the cost of their services.
The issue is this: costs for services in the USA are regulated by hospitals. And while in other developed countries governments, insurers, and private firms make them keep the prices in a reasonable range, in the USA people may pay $1000 for asthma respirator.
Statistics show that healthcare services’ conspire the largest part of healthcare expenditures - near 69%, efficiently beating even drug prices.
While current government strives to create good opportunities for businesses, businesses are doing what some providers aren’t, fuelling the market with affordable, accessible care services of high quality. That's part of the reason why the USA is considered such a good option for digital health businesses and new startups: there are lots of issues to be solved.
Subscribe to our newsletter to receive articles about digital health technologies and their application in healthcare.
Tell us about your project
Fill out the form or contact us

Tell us about your project
Thank you
Your submission is received and we will contact you soon
Follow us
