

Virtual and augmented reality in digital healthcare
The digital healthcare industry evolves fast, especially as the 2020 pandemic forced institutions to increase quickly increase medical research speed and efficiency and adopt remote healthcare services. Specialized care delivery facilities are on the rise. New trends in healthcare, such as telemedicine, self-monitoring, and distant consulting, advanced significantly. Software development for the healthcare industry created numerous jobs and implemented tools to ease patients' lives.
Among these tools, there is virtual and augmented reality for healthcare. Augmented reality (AR), which creates an interactive experience of a real-world environment through computer enhancement, and virtual reality (VR), which simulates real-world experiences fully, have already been utilized in over two dozens companies that now test their limits and usability. Let’s talk about the benefits and limitations of VR and AR in digital healthcare.
What companies already implemented AR and VR in their practices?
Goals of businesses that are already using AR and VR in their research is to find out all practical fields where they can be implemented.
AR can model a computer-generated human body for clinicians to study and analyze without worrying about causing harm and possible errors (and making errors teaches them to know them and avoid them in the real settings), so it’s a promising technology that can assist new medical practitioners in learning. That’s what Augmedics, a US-based company does; their focus is spinal surgeries that require high precision and skill, and 3D presentations of patient’s autonomy enable the surgeons to find pathologies based on X-ray vision. Experts at Augmedics consider their research to be the future of the healthcare industry due to their AR-based navigation technologies.
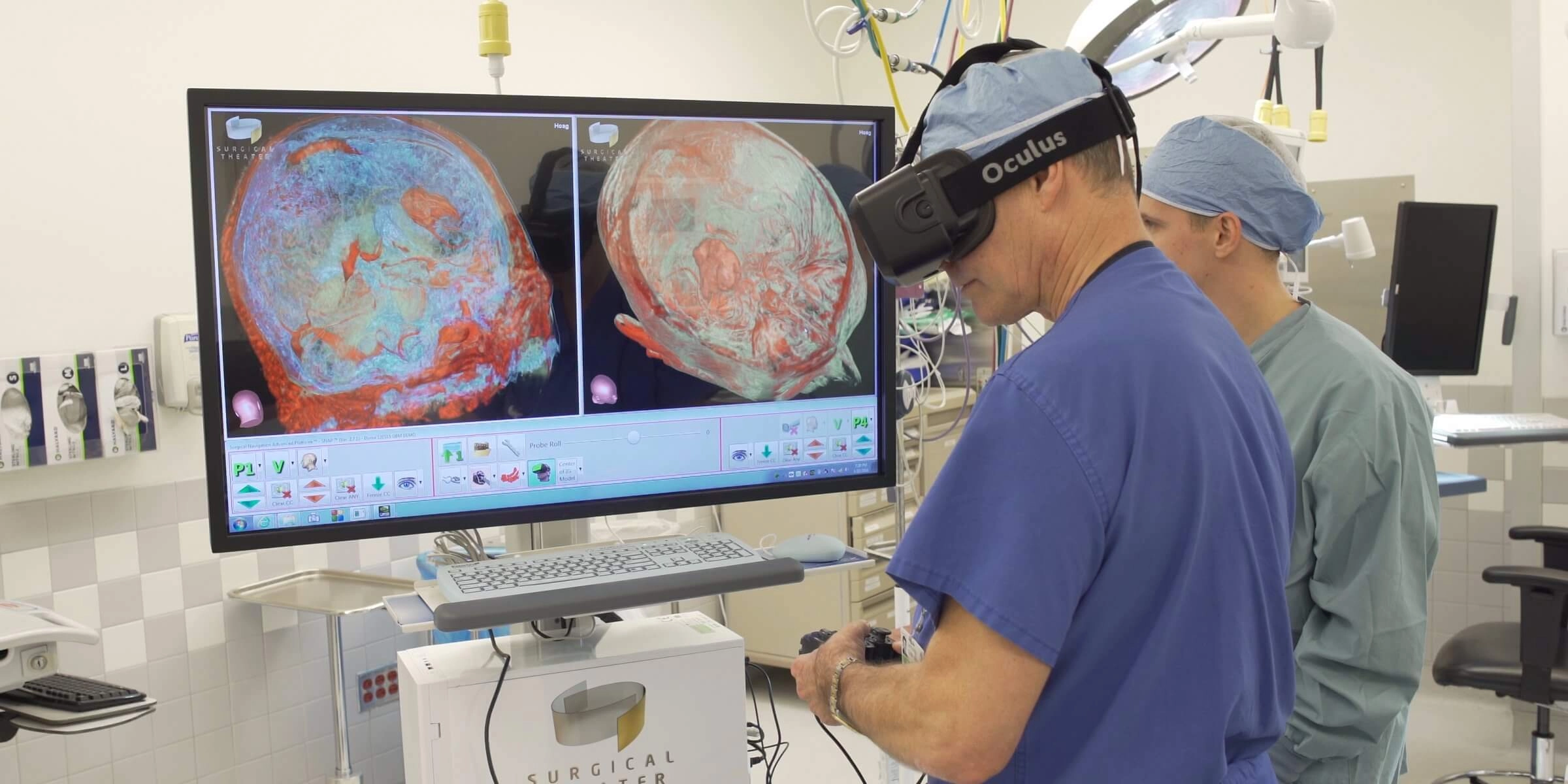
Similar opinions express Surgical Theater, which uses VR in healthcare as a surgical simulator. Their platform Precision VR provides visualization of a patient's body that surgeons can research and study long before the operation. They partner with professors and students from the University of California, Los Angeles (UCLA), New York University, University Hospitals Case Medical Center, Mayo Clinic, Mount Sinai, and Stanford University to create enhanced simulated human-body models for anatomy studies and medical training and test them immediately. After the testing, healthcare organizations and other businesses can use scholarly-proven and pre-tested models for their projects.
Similar services are provided by FundamentalVR, the UK-based simulation platform that aims at training surgeons for stressful and difficult operations. From their perspective, healthcare in the future is likely to excel at remote operations through the mix of AR and VR technological advances. Their HapticVR allows surgeons to physically touch the patient's body through haptic gloves. This means that medical companies perceive VR as more than a temporary trend that will likely fade away. Despite limitations to their research, HapticVR will likely be the best training tool for inexperienced anxious surgeons and don’t feel confident.
Successes and issues of AR and VR in clinical use
According to Healthcare Magazine, VR already assists patients in pain reduction and improves their mental health. A 16-months study at Applied VR revealed that 3D nature videos reduced patients' feelings of anxiety, psychosomatic pains, and overall pain scores.
The research has been performed based on Cedars-Sinai Medical Center along with Traveler Insurance, Bayer, and AppliedVR. According to their findings, virtual reality has another benefit for clinical use: addressing mental health issues. In particular, they focus on PTSD assistance for the retired military and similarly vulnerable patients. Additionally, the technology can help the US opioid crisis that swept the country due to the COVID-19-related depression.
Another possible success of VR clinical use is remote rehabilitation programs. VR-based treatment programs for upper extremity and lower back chronic pain are proven efficient for training at home. Karuna Labs, the leader of VR-assisted rehabilitation programs, is currently working on expanding its therapeutic programs beyond chronic pain management. Their goal is to prove the virtual opioid-free programs' superiority over conditional ones using remote training and research.
Still, virtual reality and healthcare do not partner so well as one would hope. The research of Jennifer Silva, MD, shows that VR should not be rushed into cardiovascular medicine. The barriers to its adoption are motion sickness and aberrations in surgeons’ perception of the actual patient’s body. In the healthcare industry, the process of AR and VR adoption is slow and should be handled with care and balance in mind. Dr. Silva thinks that the trained surgeons should not re-teach themselves to use virtual reality as the technology can disrupt their skills and be, in general, quite confusing. Such issues in training, along with bulky equipment, and the lack of physical contact are barriers that, while temporary, but significant and require a lengthy adoption period. The experienced surgeons may find it difficult to adapt their knowledge to the specifics of virtual reality and remote surgeries.
What are the limitations of AR and VR accuracy?
The concerns expressed by Dr. Silva are not groundless. The major obstacle to the full implementation of AR and VR in future healthcare delivery is its varying accuracy.
VR might become a regular surgical planning tool, but it really falls behind as a remote surgery technology. AR’s use is limited, too, as its best fit is an optimization of working with the electronic medical record system.
Medical precision of these technologies is currently dependent on numerous factors, such as:
- motion sickness,
- 3D modeling' refinement,
- electronic health records integration, and
- AI's limited ability to model the situation
Another limitation is the lack of physical contact. Often, an experienced surgeon can find the problem much faster without any VR model. Moreover, they can quickly react if the patient’s state worsens—but it’s hard to do so working remotely via VR. Even if the medical practitioner is near the patient, the “perceived distance” between them is one of the major concerns for remote VR-related research because it is difficult to measure the difference between the virtual environment and the real one. As Oman Medical Journal suggests, other associated challenges include safety concerns, design issues, and possible side effects as well as the current lack of regulation to ensure compliance and patients’ safety. More research is needed to prove the reliability of the technologies. Lastly, the very architecture of clinical models might not be applicable for sensitive surgeries such as brain surgery or tumor removal. Healthcare providers should treat AR and VR with caution and strictly regulate their usage.
Conclusion – temporary trends or the future of the industry?
AR and VR use in clinical practice are not just a temporary trend. These technologies’ success in mental studies, medical training, and surgery planning is highly valuable. They have already contributed to the clinical practice without any significant risks for the patients.
VR-assisted human body models enhance the studies of surgeons and AR allows immediate merge of different parts of the clinical patient record into one highly customizable, easy-to-use, accessible system.
Still, VR and AR use should not be overestimated as, in many cases, their implementation is limited due to the risks posed to the patient's life and possible hidden technical errors.
So, answering our headline question: while both AR and VR are the future of medicine, these technologies need to improve and currently cannot be used as a reliable tool for medical intervention.
Tell us about your project
Fill out the form or contact us

Tell us about your project
Thank you
Your submission is received and we will contact you soon
Follow us
