

How to Build Easy-to-Use EHR System for Hospitals
According to ACHP survey, conducted in 2016, 99% of the USA hospitals use some Electronic Health Record (EHR) system — and these systems contain health data on more than half of American population. For outsiders, such numbers seem like a pretty good opportunity to enhance data analysis and improve decision-making in health organizations. Yet, the press is full of disappointed voices telling how infuriating it is that computerization is standing between physicians and their patients. Is that a buzz or care is really getting out of care providers’ hands? What vendors can do to improve the patient-doctor relationship and enhance patient care? We’ll answer the question later in the article, but first, let’s kill terms confusion and review the overall state of EHRs in healthcare.
State of clinicians’ relationship with EHRs
Electronic health records (EHR) is “systematized collection of patient and population health information in digital format.” Clinical data in EHR includes information on patients’ medical history, their lab results, vital signs, personal demographics, allergies, vaccinations, etc. “EHR” is often used interchangeably with “EMR” (Electronic medical records), but some professionals distinguish EHR as a comprehensive system with patients’ data and receipts’ information and EMR as a collection of unstructured digitized medical records. We’ll be using the term “EHR” only.
On the contrary to the buzz about bottlenecks in digitalization of hospitals, according to National Physician Poll, 63% of physicians think EHR implementation improved patient care and they are “at least somewhat satisfied” with their systems. And yet, EHRs, despite the fact they’re promoted as a software that helps hospitals make better decisions and optimize healthcare processes is viewed as a simple data storage. Moreover, instead of timesaving features that EHR vendors’ marketing usually articulates, most physicians feel the increase in their daily basis and more than half of their “patient time” they spend working in a system.
Which is not good. So: doctors don’t hate EHRs. They just don’t see its clinical effectiveness. They also think EHRs’ interface is pretty rigid and not clear — which explains a lot of wasted hours. 72% of physicians want to reduce the amount of not useful/impactful interactions and reduce screen time.
Act on what “intuitive design” and “good user interface” mean for your end users
We’re trying to get rid of terms that produce more uncertainty than certainty, so let’s face it: design can’t be “intuitive” because “intuition” is a characteristic of users, not of products. For users to be intuitively sure when to press this button and where that links, the design should be recognizable and clear. In other words, it should cause the thought “Oh, I know how to use it” or, at least, “Oh, it doesn’t look complicated, I’m sure I can figure it out”.
One of the main barriers between physician and EHR vendor is that the latter doesn't really involve in the patient care workflows. Most physicians from Stanford University survey believe that EHRs need a complete overhaul and 31% agree that software development companies that create EHRs don’t particularly care about user experience. So, to make users intuitively — quickly and with minimal confusion — recognize elements in your EHRs interface and use them comfortably, you have to talk with them, conduct user research, and then test rigorously.
Note, that when conducting research you need to ask questions about interactions with EHR at the point of care delivery to different patients, for instance:
- How will you use EHR if there’s an emergency in your patient? (or “Will you..?)
- How are you preparing to recurring appointments?
- How are you preparing for the first appointment? etc.
- What data specialist in X area of expertise wants to see interacting with patients with X1 diseases?
A poorly constructed, generic interface most physicians are talking about makes completing clinical tasks within EHR a very challenging process. That is why we advise software development companies to hire people with a medical background in their product teams or at least consult them regularly: if you don’t know where dentist looks to re-evaluate her analysis of X-ray photo, for instance, you can’t build a proper user flow for her, etc. It’s better to get some help.
Create a customizable, modular dashboard
One of the EHRs’ specifics doctors are dissatisfied the most is the inability to change the system accordingly to their liking. Despite the fact that all EHR must contain a certain amount of features to be compliant to HI7 and ISO standards, there is still an option to give users the possibility to regulate which info about patients they want to see while working with a system and which are unnecessary to them. Interfaces are as good as they are capable to meet their users’ needs and adapt to them.
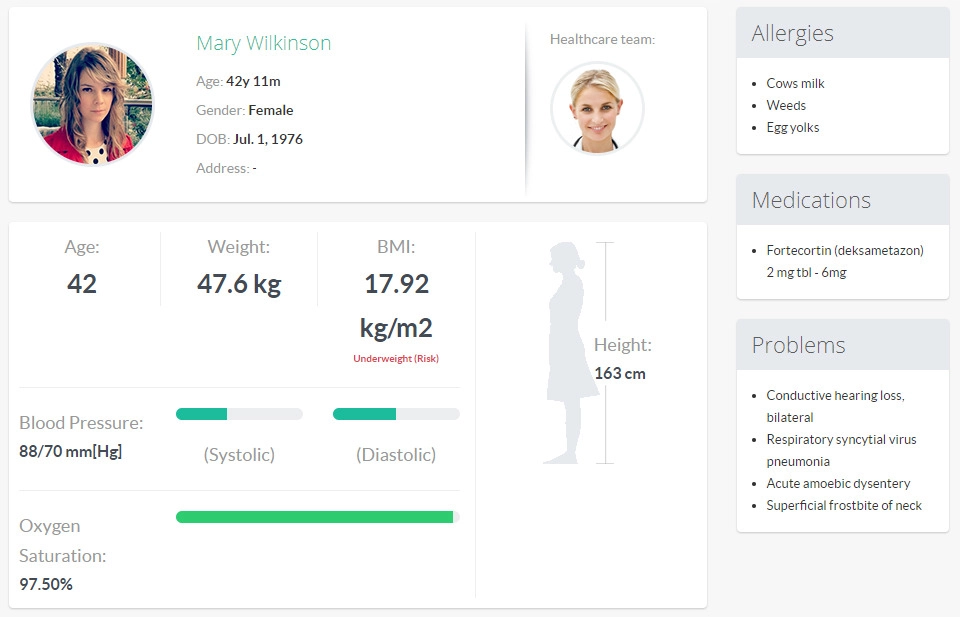
Aside from the option to regulate physicians’ own “data preferences”, you can pre-prioritize data in the system accordingly to doctors’ role and practice stated in their profile.
Introduce a clear timeline in patients’ data
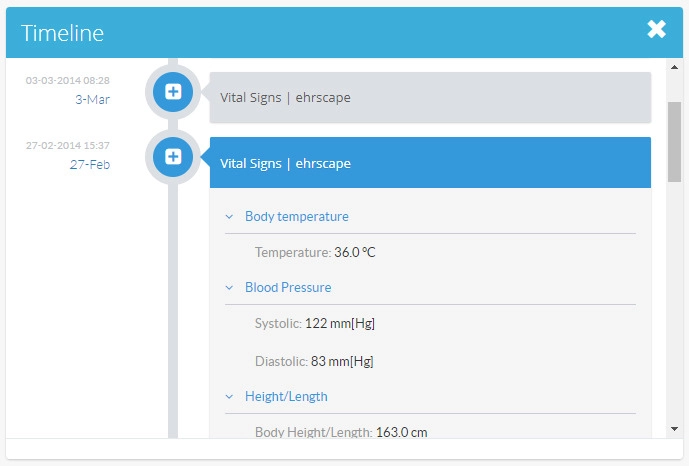
Doctors want to see consistency and clarity when working with patients’ data, and timelines with understandably structured vital signs, lab results, and summaries of the previous appointments are an important part of that consistency. Don’t forget to add segmentation by type of doctors’ practice and introduce reports on how patients felt in a defined period of time (within a week, months, etc.) It would better if the structure of the timeline will be prepared to transmit a constant flow of real-time data: the rise of wearables in the healthcare slowly continues and doctors are waiting for these devices, too.
Plus — let’s touch the subject of interoperability briefly — timeline feature might be integrated with larger datasets from patient health monitoring. Then, physicians will be able to compare how patients feel with how people feel generally, epidemic outbreaks, closing or opening of other health facilities (or algorithms will do it for them). That will allow clinicians to understand root causes of patients’ conditions deeper, and hospital management, on the other hand, will be able to prepare for the increased level of visits.
Voice recording / Scribing technology
79% of physicians are entering their notes into EHR manually, right in the middle of the appointment which results in lesser time spent with patients. Voice recognition software is what would help doctors to spend more time with patients than with a computer. Which is very important, both in terms of patient satisfaction and in terms of doctors’ engagement in their work duties. Healthcare is an industry where people work to help other people. When the time is taken from them and dedicated to other, often non-clinical, activity, they don’t feel their work is of any value. Even in terms of distraction management, constant interactions with EHR is something that doesn’t help doctors concentrate. And hey, the focus is what vital for them.
Use language people speak
We won’t elaborate on this one too much, just take a look at this picture.
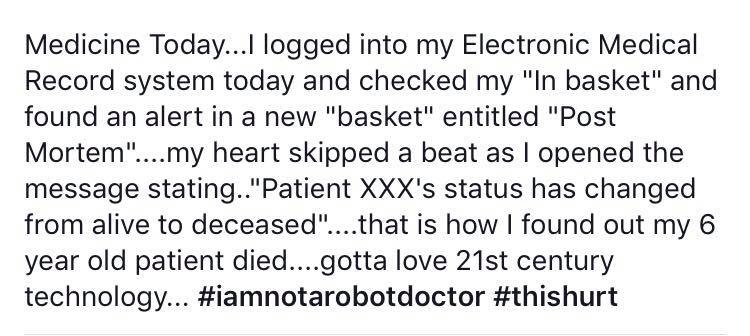
Hands-on decision support
Another helpful, from the clinical effectiveness point of view, the feature would be to implement data science algorithms that connect current symptoms in patients and their previous lab results, vital signs, and other physicians’ notes, showing the correlation in the form of tooltips or notifications.
Doctors also would like to see advises on how to manage patients with complex conditions and get alerts and reports on high-risk patients in the portal.
We’ve already said that it’s important to introduce algorithms that work smoothly and quickly to provide physicians with recommendations when they need it the most. EHRs consist of structured and unstructured data, and if it operates within a large hospital network there are tons of them. Unsupervised machine learning algorithms built by an expert data scientist with healthcare expertise can help to gather valuable health insights from the latter.
Take steps to improve patient-doctor interactions
Doctor want EHRs and other digital tools that are used in hospitals to be helpful in their work, not distract them from what they have to do. What, except for design interactions optimizations, EHR providers can do to improve their relationship?
Provide patients with access to their medical and financial data
You can create a new type of profile for patients and invite them to EHRs system — or you can create a mHealth app that will receive updates on appointment conclusion, lab results, show doctors’ notes to patients, etc. People want to review and control their health data, that gives them control and understanding of what’s going on with them.
Doctors also want EHRs to show patients their financial information, so they’d understand what are they paying for and have the ability to choose the most suitable care options.
Connect them via chats or telemedicine
Doctors vote for the development of mobile apps, integrated with EHRs, both for them and for patients partially because it's an opportunity to reach their consumers and improve the quality of care. Via communication tools, physicians would be able to educate them, calm them, increase awareness of possible health issues or of recent developments in public health. So, if there’s a possibility to build a bridge between patients and providers within EHR, do it.
Introduce online scheduling
Both patients and doctors want to manage appointments online, so it’s a good idea to consider this feature, too. We’ve described best practices for building mHealth scheduling solutions here.
Address hospital management issues
According to this research, while “some functions sufficient and suitable for many users, but it seems it is not for nurses and physicians.” It would be safe to say that EHR is a business or an administrative tool, than a tool that can be used for clinical tasks. Another way of fixing that is by addressing interoperability issues, both within one care facilities and between different providers.
Introduce real-time data entry for all care specialists
“All” includes nurses, physicians, lab staff, — everyone involved in the care process. Live data charting and smart alerts are challenging features to implement and right now nurses feel like attempts to implement them only add more time to their shift. But, if an interface is modeled in order to be consistent with different departments’ expectations; alarms are prioritized; voice recognition software works more or less flawlessly; there is a possibility to transform EHR from time-consuming headache to useful hospital management tool. The key here is, again, run as many test scenarios of using EHRs as possible, and talk to as many people, involved.
Establish communication between departments and between different health providers
Include options to share patients’ data and thoughts. People with different experiences make a better decision, teamwork is often more productive and resultative than “I always work alone” mode. Include commenting feature on lab results, X-ray, MRI photos, etc.
Add to your EHR self-management and learning tools
If you want your EHR to empower doctors, address not only features that improve their clinical practice, but also options to organize and control their time. It could be a notebook, or algorithms that will show them recent clinical studies and research in their field, it could be a financial management tool or even an e-learning portal.
Secure your EHR (!)
EHR is a software where people constantly add data and the ability to receive data is also a risk to receive a virus or injection. In February, one hospital in Columbia reported a security breach that affected 400 thousand patients. The overall level of hacks, breaches, and leaks within EHRs is tremendous which means a) startups and software development companies don’t consider all specter of human error possibilities, b) there’s not enough training for hospital staff, c) the system itself isn’t protected properly. When hospitals started to shift medical records to the cloud, the number of breaches increased. The industry that has a significant influence on human life and death is better not to be disrupted.
As a software provider, you should consider how to protect your system from breaches. You must have established cybersecurity strategy, algorithms to track attackers and mistakes and block inconvenient, doubtful input. Your EHR must be HIPAA compliant. Notifications about something is happening are also a must. Sensitive patients’ data must be encrypted, no matter where it is stored (even if it’s in transition). Educate hospitals (CEO, clinicians, their patients — if they have access to EHR, everyone) on passwords policies, access to accounts, and provide them with comprehensive training.
And how is that easy to implement? Briefly on adoption strategy
If you want hospitals to adopt EHR productively, first, know if they have processes to adopt changes. Focus on a few hospitals and become a loved guest there. Get familiar with the medical workers. Learn if they would implement some changes in their workflow, what EHRs are they using right now, how the previous adoption went like. Surely, it’s a process that doesn’t scale, but if you want a product that won’t get a "parody Twitter account", deep research will be pretty much helpful. If you don’t have time for this and you’re not sure if a hospital has a framework for change, make one and add it to your solution.
Second, a research found 54% clinicians believed their workflows were no better than before the EHR, so introduce training materials that are easy to understand. Note, that learning is more effective if it’s closely followed with practical tasks. Don’t forget to provide hospitals with support and maintenance services and start small.
We think, one of the main issues with healthcare providers—HIT (health informational technology) vendors relationship is a huge gap between them. Startups and software companies happen to talk to stakeholders that don’t usually interact with patients. Stakeholders make a decision based on the risk-benefits evaluation. Physicians are left behind the whole process, and, as a result, the hospital is forced to reduce the amount of time for patients to take time to learn how to use an EHR. Cost loss and patient dissatisfaction is a result. You can change that.
Tell us about your project
Fill out the form or contact us

Tell us about your project
Thank you
Your submission is received and we will contact you soon
Follow us
