

Medical Imaging Solutions: PACS, VNAs, and a Migration Challenge
The healthcare industry is a bearer of tons of data about human health, imaging data is prevalent in the list, and its amount in 2019 is growing. Models for 3D printing, CRISPR-driven genome imaging, and so on — the more wonderful advancements healthcare and technology make, the more pictures are being made. How the industry handles these pictures? Let’s take a look.
DICOM and PACS
With digitization and spreading of EHRs use, medical institutions kind of elevated the level of medical image management. Eventually, professionals across the world came up with specific, standardized systems to store and transmit imaging data.
DICOM (Digital Imaging and Communication in Medicine) is the universal standard for, as you’ve guessed, communication and management related to medical images, rules of their storage and transmission. According to this standard (which consists of so-called services), all the data in the .dicom format — have to be stored at PACM.
PACS (picture archiving and communication system) is an imaging storage technology that helps to access and transmit DICOM files — aka X-ray films, MRI images, and so on. Radiologists came up with another acronym — RIS (radiology information system) — which became a core system for management of imaging department that includes scheduling, performance tracking, and even billing. A system was complimentary for PACS.
Main parts of a PAC system will be
- Hardware that produces medical imaging
- A network where data is transmitted and shared
- A workstation
- And, finally, the archives where imaging data is stored and where doctors should go for retrieval or relevant documentation
Medical workflow started to rely on these systems heavily: through RIS radiologists sent transcribed results, through PACS they shared images — people from other disciplines that use imaging diagnostic did so as well. Specific, shaped to be compliant in the healthcare ecosystem standards now used worldwide.
PACS challenges
Challenges, predictably, occurred, and the reason for that was growth: both of the healthcare industry and of software vendors. The industry required more storage and wanted to try new technologies, provided by different vendors.
Migration between PACS vendors was extremely time-consuming and often insufficient. But it occurred that the migration from one PACS vendor to another meant changing and preparing the data for migration — different technology vendors applied DICOM syntax differently, so one MRI image from one system often didn’t open up in another. The process was rather rigid and time-consuming.
PACS data updating and processing were also very long. It was tedious to update the archive with new research or retrieve some old images. That basically meant two things: patients waited a lot if they were to retrieve their old MRI scans — and data in there, being inaccessible in a timely manner, couldn’t be used for research and analysis purposes.
One image at the time, on a dedicated scanner/clinical viewer. Also, often PACS solutions allowed doctors to see only one image at a time — and only on dedicated screens or scanners. Which damaged their ability to make a comprehensive, throughout diagnosis, and, therefore, affected health outcomes.
Different departments had different PACS software. That greatly affected enterprise collaboration, and productivity wasn’t sustainable in terms of cost-effectiveness and had an impact on patient outcomes.
Healthcare organizations still use PAC systems — we’ll talk about why later on, — but now they are more and more often considered as legacy systems (at least, in theirs “not upgraded” look).
Now, about these upgrades.
Vendor-neutral archives for medical imaging data
The concept of VNA was proposed to eliminate the collaboration-between-department-is-absent challenge.
VNAs or Vendor-Neutral Archives are multicenter and multi-enterprise archive systems, but they accept and transmit imaging data from any vendor, wherever the data came from. VNAs also stores DICOM files but they also connected departments within organizations, whatever PACS they were using, and more or less severed data migration issue.
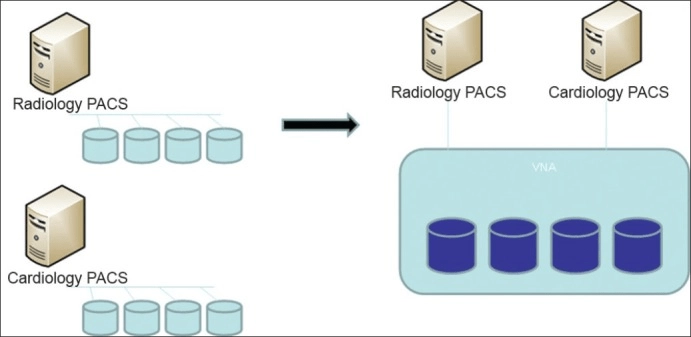
Basically, VNAs allowed what PACS couldn’t: they removed the dedicated scanners from the equation and let doctors store and share images everywhere they like (like, on a laptop, and a smartphone). VNAs also can be stored on whatever HIPAA-protected storage an organization wants it to store — for instance, in a cloud. It’s a smart medical archive that can be connected to several PACS and process DICOM and non-DICOM files. PACS, though, is more of a viewing and storing system for medical images.
Plus, VNAs allow easy updates on changes in patients’ status if patients aren’t doing any imaging tests — and they compress their data.
Different VNAs solutions include dashboards that present patients’ imaging data and other PHI for comparison, some of them are modular and customizable — they even can be integrated into managing platform or EHR to merge different aspects of clinicians’ workflow.
PACS to VNAs: the question of migration (or transformation)
To migrate or not to migrate? Basically, PACS alone are outdated, thus the answer to this question should be obvious. But, as usual, it’s not that simple.
Cost-effectiveness is looked forward by every business, and migration to VNA is costly.
Migration is, itself, a tiresome process — even with usual files— but with DICOM files the complexity is higher. Files in this format contain metadata with patients’ personal information that is separated from the image, itself, a location pointer, that is also assigned to an image but isn’t actually connected to it. So, during migration, organizations need to ensure every part of the trio is migrated correctly and conduct audits and acceptance tests afterwards. So, it’s time-consuming and expensive.
Significant positive effect on business outcomes lays in three-five years, which makes migration from PASC to VNAs a rather hard decision.
PACS, though, is the right solution for small clinics that offer targeted expertise, without a variety of departments and professionals from different fields — for a dentist office, for instance. Some PAC storage systems now capable of processing none DICOM files, and they are more affordable in comparison to VNAs — which is important if an organization is small or young.
But. Right now, 3D image/display radiology solutions are installed in more than 40% of American hospitals. The remaining 60%, most likely, have PACS installed. Think about the influence such transformations make, in terms of efficiency of healthcare — in large enterprises.
Organizations begin to understand that silos in their infrastructure slow them down, so the accessibility and interoperability between different departments become a must. As well as the agility of care delivery and data retrieval.
Tell us about your project
Fill out the form or contact us

Tell us about your project
Thank you
Your submission is received and we will contact you soon
Follow us
